Background
Dr. Salvatore Zavarella is a distinguished board-certified Long Island neurosurgeon with over 15 years of experience. He practices at NeuroCare Long Island, a leading neurological center under the umbrella of Northwell Health. Dr. Zavarella specializes in complex spinal surgeries, minimally invasive neurosurgical techniques, and the treatment of brain tumors. He is renowned for his patient-centric approach, combining advanced medical knowledge with compassionate care.
The Case of Patient D
Patient Profile:
- Name: Patient D
- Age: 23
- Occupation: College Graduate
- Medical History: Adolescent scoliosis diagnosed approximately 10 years earlier
- Symptoms: Persistent localized pain in the lower thoracic and upper lumbar spine, worsening with activity and prolonged positioning.
Initial Consultation
Patient D presented to the office with worsening pain localized in the lower thoracic and upper lumbar regions of the spine. The discomfort was non-radicular and primarily affected the parathoracic and paralumbar areas.
The patient reported that the pain had gradually worsened after finishing college and was particularly aggravated by physical activity and prolonged sitting or standing.
She had originally been diagnosed with scoliosis during adolescence approximately 10 years earlier. At that time, she underwent bracing treatment around the ages of 14 to 15. However, she was unable to tolerate the brace and discontinued treatment. After completing her growth, her symptoms initially improved, but over time the pain gradually returned and intensified.
Conservative Treatment
Prior to considering surgical intervention, Dr. Zavarella recommended conservative management.
The patient underwent physical therapy along with specialized scoliosis rehabilitation known as Schroth therapy, which she had previously attempted earlier in life. Despite these efforts, the patient experienced minimal improvement in her symptoms and continued to experience persistent pain and functional discomfort.
Diagnostic Workup
Dr. Zavarella ordered a comprehensive radiographic evaluation to assess the patient’s spinal alignment and determine the appropriate treatment plan.
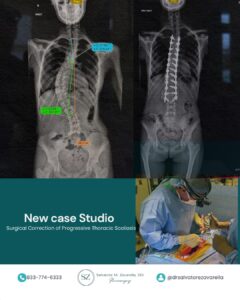
X-Rays of the Spine revealed a thoracolumbar scoliosis curve measuring approximately 35 degrees.
Additional curves were also identified:
A proximal thoracic curve measuring approximately 7–8 degrees
A distal lumbar curve measuring approximately 19 degrees
To evaluate the flexibility of the spine and guide surgical planning, bending films were obtained. These studies demonstrated that the proximal and distal curves corrected nearly to normal alignment during bending, indicating that they were flexible compensatory curves. However, the primary thoracolumbar curve remained partially rigid, correcting only to approximately 17–18 degrees.
Treatment Plan
Based on the imaging findings and the patient’s persistent symptoms, Dr. Zavarella recommended surgical correction of the primary structural curve.
Because the upper and lower curves were flexible and corrected well with bending, Dr. Zavarella planned a selective surgical approach that would address only the primary thoracolumbar curve while preserving as much natural spinal motion as possible.
Surgical Procedure: Selective Thoracolumbar Instrumentation and Fusion
Dr. Zavarella performed selective instrumentation and spinal fusion from T8 to L3 to correct the structural thoracolumbar deformity.
Preoperative Care: The patient underwent a complete preoperative evaluation including imaging review, laboratory testing, and anesthesia consultation to ensure surgical readiness.
Surgery: During the procedure, instrumentation was placed from T8 through L3 to correct the primary thoracolumbar curve. This selective approach allowed the surgical team to stabilize the structural portion of the deformity while maintaining mobility in the surrounding segments of the spine.
Postoperative Care
Following surgery, the patient was closely monitored during the postoperative recovery period. Imaging confirmed a successful correction of the primary curve and proper spinal alignment.
Postoperative X-rays demonstrated an excellent lateral spinal profile, with a smooth transition between the thoracic and lumbar spine and preservation of normal lumbar lordosis.
Follow-Up and Recovery
During follow-up evaluations, the patient demonstrated significant improvement in spinal alignment and overall comfort.
As expected with selective correction:
The proximal thoracic curve spontaneously corrected to normal alignment.
The distal lumbar curve improved significantly, decreasing to less than 10 degrees.
Long-Term Outcome
Following surgery, the patient reported a significant reduction in pain and a noticeable improvement in her quality of life. By addressing only the structural portion of the deformity, the procedure successfully corrected the spinal imbalance while preserving natural spinal motion and mobility.
Both the patient and the surgical team were very pleased with the outcome.
Reflections and Conclusion
Dr. Zavarella’s management of Patient D’s thoracolumbar scoliosis demonstrates the importance of individualized treatment planning and the strategic use of selective spinal fusion techniques.
By correcting only the structural curve while preserving flexible segments of the spine, Dr. Zavarella was able to achieve excellent spinal alignment, reduce pain, and maintain functional mobility.
This case highlights the effectiveness of modern spinal deformity surgery and reflects Dr. Zavarella’s commitment to delivering advanced neurosurgical care and improving patient outcomes throughout Long Island.